AARP’s Pursuit of Profits Over Patients
A PDF version of this report is available on the American Commitment website…
Some Americans might think of AARP, formerly known as the American Association of Retired Persons, as a membership and advocacy organization. However, the reality has proven far different. AARP has grown into a marketing and sales firm with a public policy advocacy group on the side. And AARP’s prime source of tax-free revenue from that marketing operation comes from its relationship with UnitedHealth Group, the nation’s largest health insurer.
For decades, AARP has been accused of questionable business practices from numerous quarters: Federal officials, who suggested a business arrangement AARP proposed (but never implemented) could violate federal criminal statutes, the editorial board of the New York Times, and former AARP employees themselves.[1] The organization’s business practices embed “royalty fees” within the premiums of those who purchase Medicare supplemental policies, called Medigap insurance, effectively overcharging seniors to fund AARP’s own operations. AARP’s revenue from these sales, and from UnitedHealth, which licenses AARP-branded Medigap and Medicare Advantage coverage, has grown year after year. Since 2007, the organization has received an estimated $6.7 billion tax-free in revenue from UnitedHealth.
As it rakes in billions of tax-free dollars in UnitedHealth cash, AARP has abandoned the seniors and vulnerable patients who have placed their trust in the organization. For instance, AARP has endorsed legislation that would effectively import other nations’ discrimination against individuals with disabilities to the United States—legislation that disability groups themselves have admitted contains serious structural flaws.
An exploration of the record shows not just that AARP holds serious conflicts of interest, but that AARP’s financial conflicts have prompted the organization to abandon its principles on numerous occasions, pursuing financial gain for itself and its partners over the organization’s stated mission and policy objectives—and its members. Congress should follow up on these facts, and its own prior investigations, by further exploring the unsavory alliance between AARP and UnitedHealth Group.
A Profitable “Non-Profit”
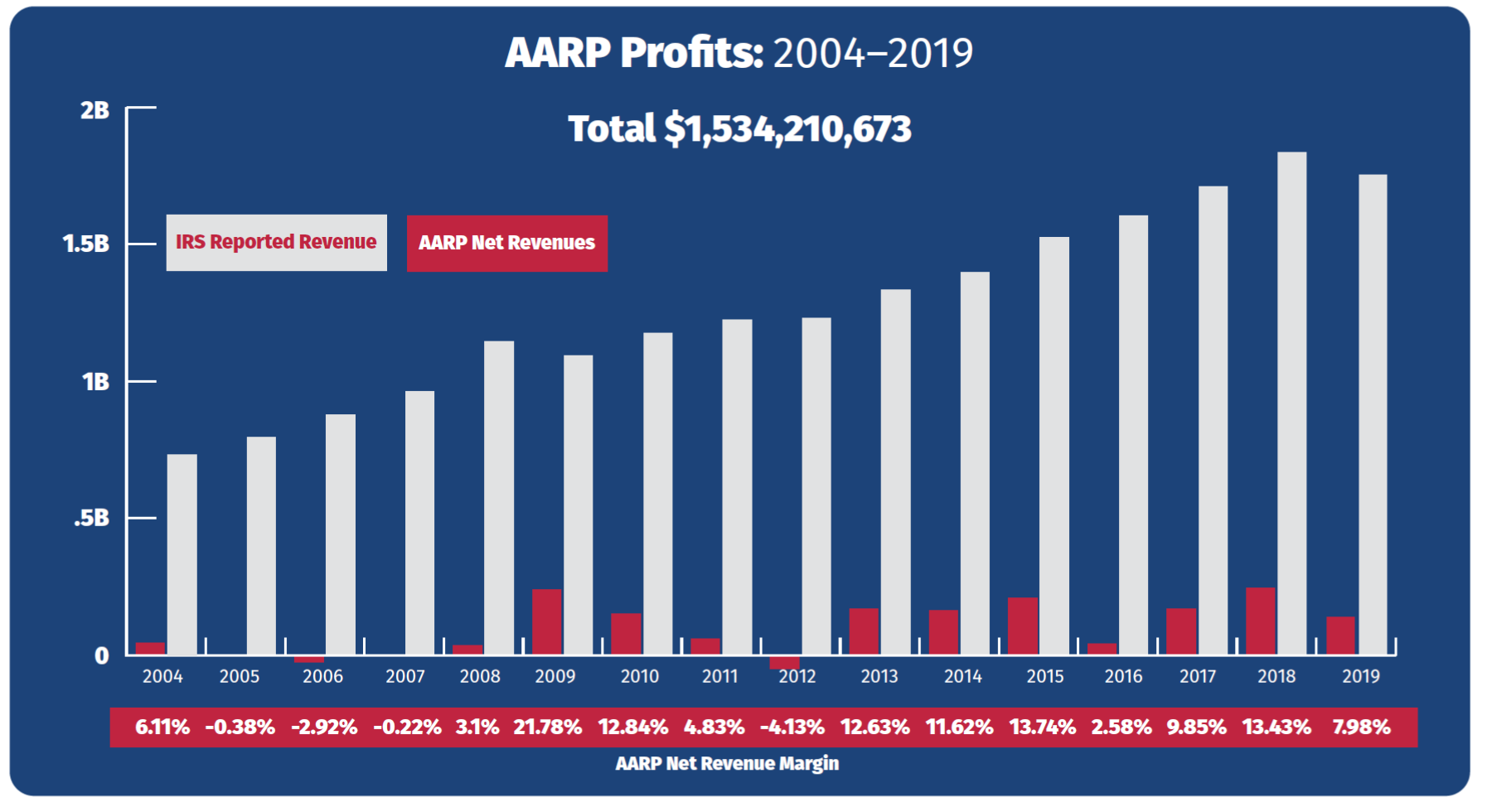
Despite the organization’s status as a non-profit tax-exempt entity organized under Section 501(c)(4) of the Internal Revenue Code, AARP has found its business very enriching indeed. According to its 2019 Form 990 filed with the Internal Revenue Service, the organization reported net income—that is, revenues in excess of expenses—of $139,791,096.[2] That surplus represents a net margin of nearly 8% of AARP’s total revenues of $1.75 billion.[3]
This sizable net income does not represent an anomaly when it comes to AARP’s fortunes. After hiring Barry Rand as CEO in early 2009, AARP converted a string of modest annual results into a series of large financial gains. Under Rand and Jo Ann Jenkins, who succeeded him in 2014, AARP has achieved a total of over $1.5 billion in net profits since 2009, achieving financial gains in all but one of those 11 years.[4] Moreover, its net revenue margin since 2009 has averaged nearly 10%, far more than the average profit margin of some industries.[5] For instance, of six health insurers listed in the Fortune 500, none had a profit margin exceeding 5.99%.[6]
A Marketing Behemoth
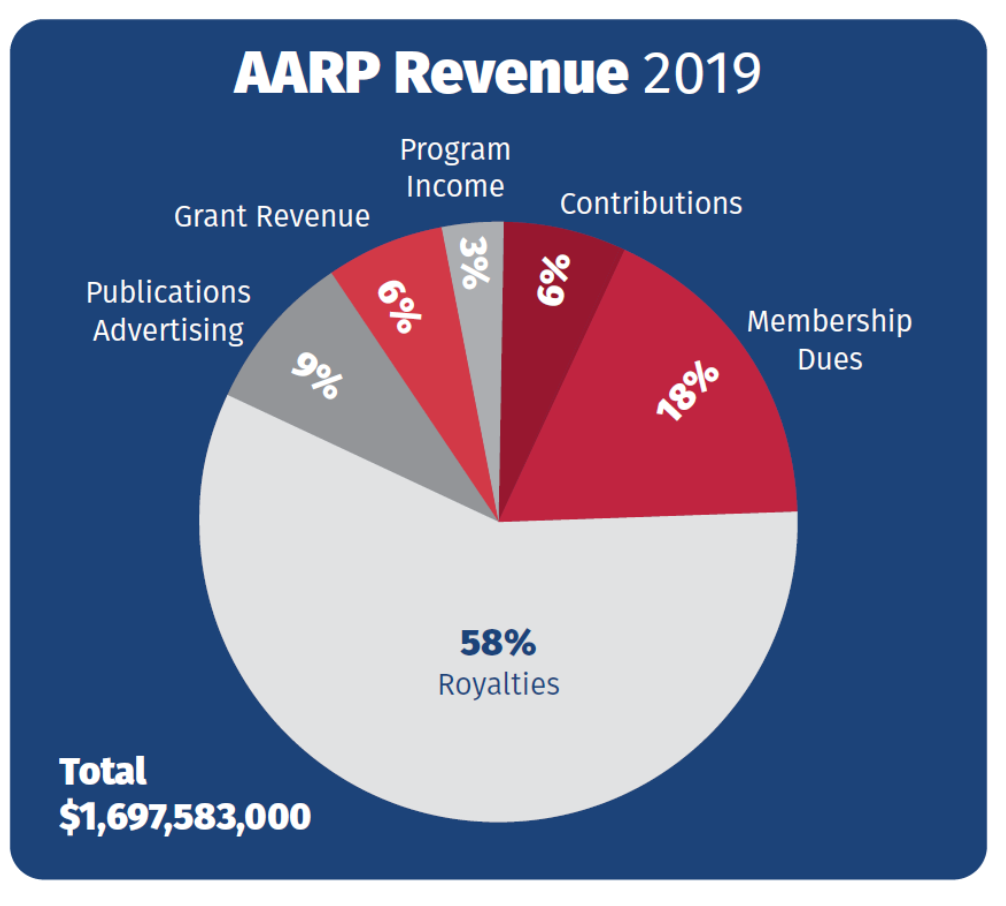
For all the revenue AARP receives from membership dues—just over $300 million in 2019, according to its most recent consolidated financial statements—the organization receives more than three times that amount selling AARP-branded goods and services to its members.[7] In fact, the organization’s “royalty fees”—which the organization claims constitute payments for the use of its logo, brand, and intellectual property—represent well over half (57.6%) of AARP’s total annual revenues.[8] In 2019, AARP received nearly $1 billion in such revenue from what more appropriately constitutes the sale and marketing of products to members, equal to nearly double the revenues generated by membership dues, grant revenue, and contributions combined.[9]
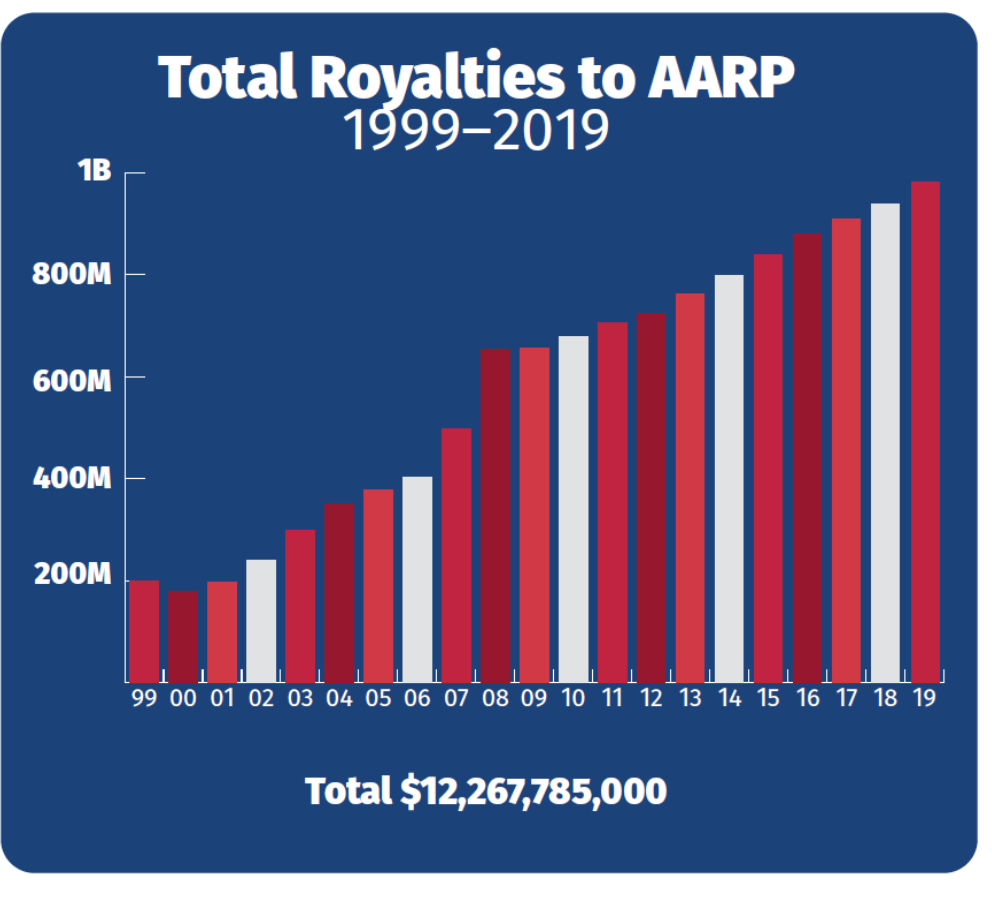
While other organizations’ revenues fluctuate from year to year, the revenue AARP has generated from selling products to its members has increased every single year for 19 years straight. Since 2000, the company’s business proceeds have increased more than fivefold, from $178.3 million in 2000 to $977 million in 2019.[10] In total, over the past 21 years, AARP has made nearly $12.3 billion selling products to its members.[11]
As AARP has expanded its marketing empire, fees from membership dues have grown at a much slower pace. While dues collections have risen over the past two decades, from $141.1 million in 1999 to $300 million in 2019, since 2014 they have remained largely flat.[12] In some years, revenue from membership dues has declined year-on-year—a contrast to the organization’s marketing arm, where revenues have increased every single year since 2000.[13]
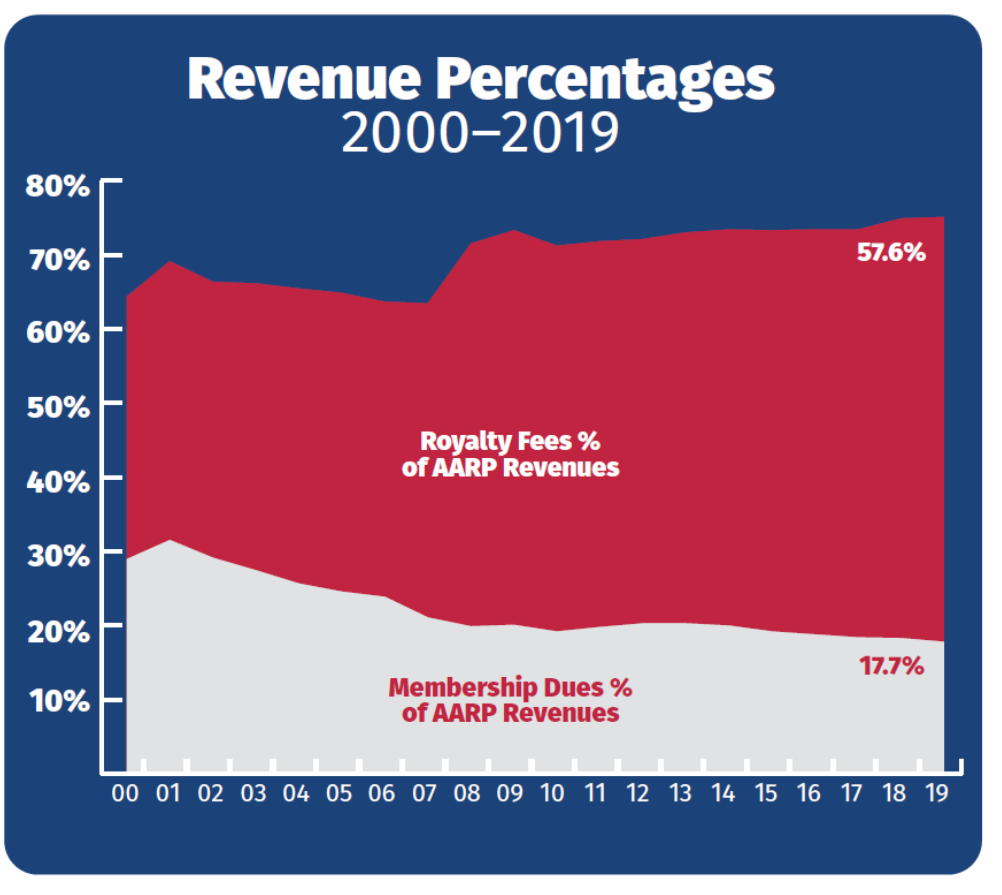
The result of the two trends—membership dues growing slowly, and royalty fees growing exponentially—has made AARP much more reliant on marketing income as a share of its overall revenues. Since 2000, membership dues have nearly halved as a percentage of AARP’s total operating revenues, from 28.9% to 17.7% in 2019.[14] Meanwhile, marketing income has grown from 35.6% of operating revenues to 57.6%, meaning AARP gets more than three times more of its budget from selling other products to members than it does from membership dues themselves.[15]
Health Insurance Business Dominates
As AARP’s sales and marketing revenue has skyrocketed overall, the percentage of that revenue coming from UnitedHealth Group has also grown. In 2007, revenue from UnitedHealth represented 57% of AARP’s marketing income, or $283.7 million.[16] By 2017, both numbers had grown substantially: Income from UnitedHealth comprised 69% of AARP’s marketing revenue and had risen to a whopping $627.2 million—more than double the amount of just a decade previously.[17]
As income from UnitedHealth Group has grown over the past decade, so too has UnitedHealth’s share of AARP’s operating revenues. As of 2017, income from the sale of insurance products through UnitedHealth exceeded income from membership dues by almost twofold.[18] While member dues comprised only 18.3% of the organization’s total revenue in 2017, UnitedHealth revenue constituted 38.2% of AARP’s operating income.[19]
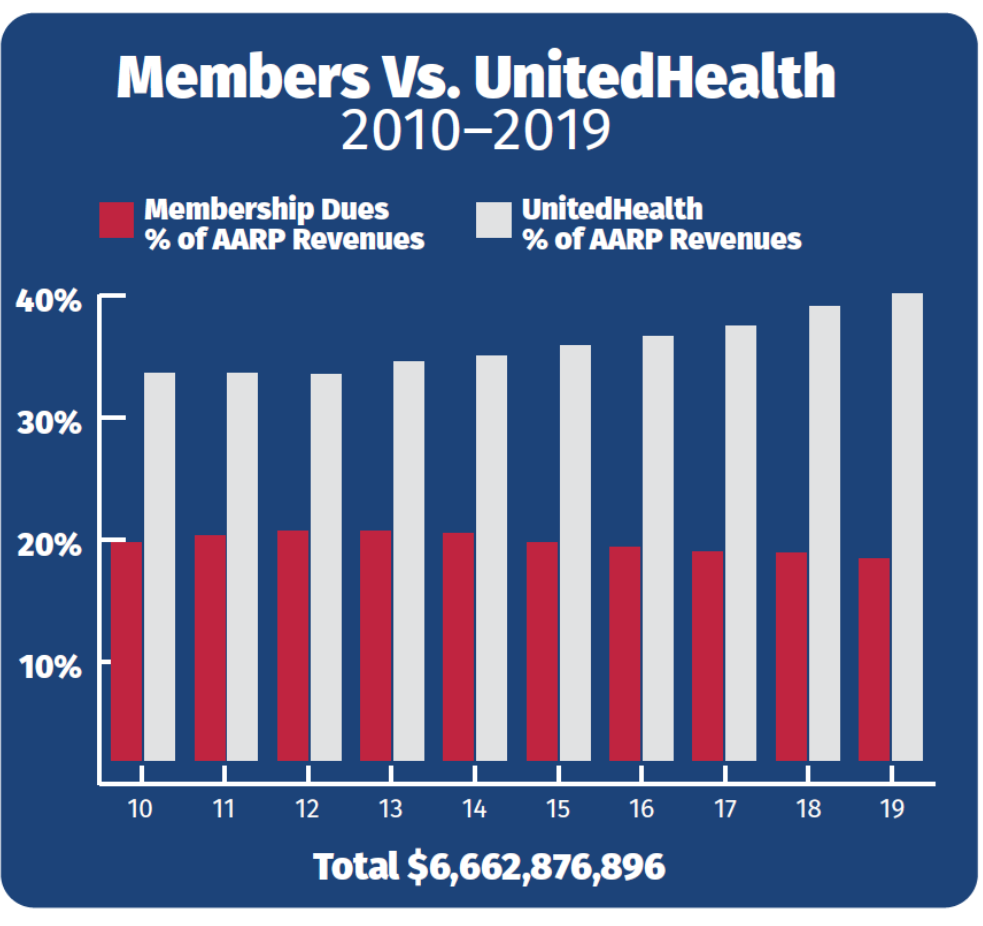
AARP’s relationship with UnitedHealth Group, discussed in further detail below, has drawn public scrutiny from Congress and other policymakers. From 2008 through 2017, AARP’s consolidated financial statements disclosed the percentage of marketing revenue coming from UnitedHealth. One could therefore easily calculate the exact amount of revenue AARP received from UnitedHealth, by multiplying total marketing revenues by the percentage of those revenues coming from UnitedHealth Group. In total, from 2007 through 2017, AARP received more than $5.3 billion tax free from UnitedHealth Group.[20]
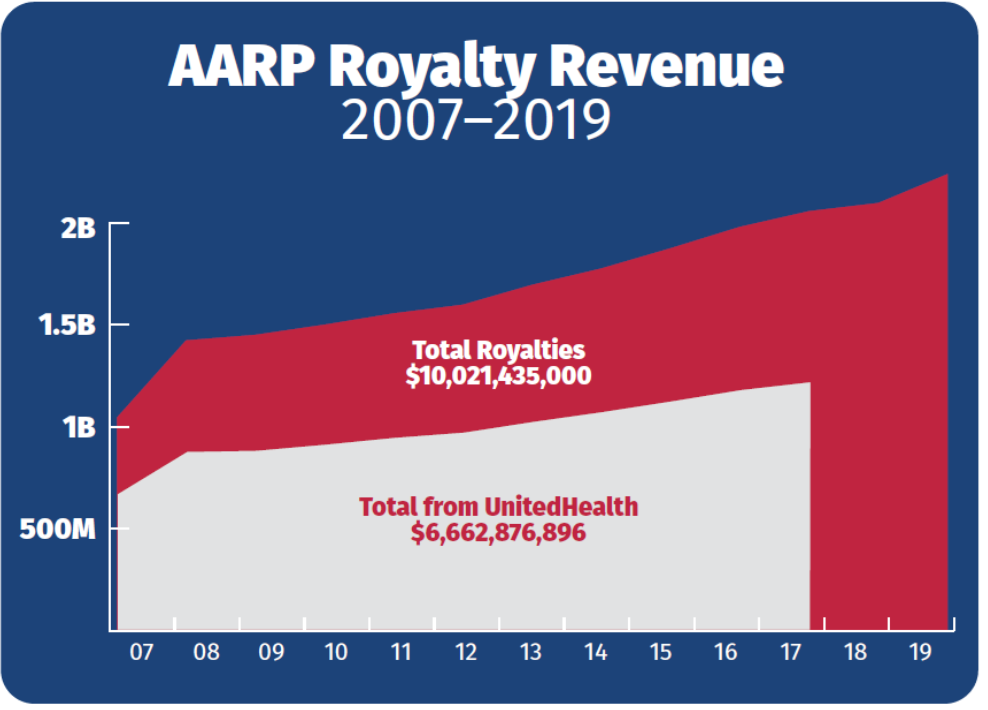
However, beginning in 2018, AARP’s consolidated financial statements failed to disclose the exact percentage of its marketing revenue coming from UnitedHealth Group.[21] Therefore, one can no longer calculate the precise amount of income AARP receives from UnitedHealth. We do know that AARP’s marketing revenue has grown every single year since 2000, and that the percentage of overall marketing revenue coming from UnitedHealth stayed the same or increased every year from 2007 to 2017.[22]
Because AARP decided to stop disclosing the percentage “royalty” revenue received from UnitedHealth Group to its members or the public—quite possibly due to increased public scrutiny over its relationship with UnitedHealth—we can no longer calculate the amount precisely.[23] However, AARP added a section to its 2018 and 2019 financial statements regarding revenue recognition, which includes an additional discussion of royalties.[24] Because information in the 2018 statements includes data for the prior year period, and because AARP did provide information on its revenue from UnitedHealth in its 2017 statements, we can create an approximation of its UnitedHealth revenue for 2018 and 2019.
In its 2018 financial statements, AARP claimed that $649.2 million of royalty revenue in 2017 came from “health products and services.”[25] In its 2017 statements, AARP noted that a total of $627.2 million in royalty revenue—or 96.6% of the “health products and services” royalties—came from UnitedHealth.[26] If UnitedHealth accounted for a similar 96.6% share of the $680.3 million in “health products and services” revenue in 2018, that would mean AARP received a total of about $657.2 million in revenue from UnitedHealth in 2018.[27] Likewise, if UnitedHealth accounted for a 96.6% share of the $716 million in “health products and services” revenue AARP reported in 2019, that would mean the organization received $694.6 million from UnitedHealth.[28]
While these numbers serve as mere approximations, they do so only because AARP decided to stop disclosing to the public exactly how much money it received from UnitedHealth Group. However, revenue in this ballpark would mean AARP received an estimated $6.7 billion in “royalty” income from UnitedHealth since 2007.[29]
Making Money on Seniors’ Money
AARP not only makes money from UnitedHealth Group—and its members—directly, it does so indirectly as well. The organization has established a grantor trust, through which it funnels payments for insurance policies issued by UnitedHealth and other insurers, including MetLife, Genworth, and Aetna. As its financial statements explain:
The [AARP Insurance] Plan, a grantor trust, holds group policies, and maintains depository accounts to initially collect insurance premiums received from participating members. In accordance with the agreements referred to above, collections are remitted to third-party insurance carriers within contractually specified periods of time, net of the contractual royalty payments that are due to AARP, Inc., which are reported as royalties in the accompanying consolidated statements of activities.[30]
In plain English, this language means that members pay premiums—including the “royalty fee” UnitedHealth pays to AARP—via the trust, and the AARP trust then pays the premium to UnitedHealth, after taking out its own “royalty fees.”
But in the process, AARP invests the funds from the day they receive the payments from seniors until the “contractually specified” time during which they transfer the payments to UnitedHealth Group and other insurers. Investing seniors’ premium payments for a short period might seem insignificant. However, given the massive sums involved—the grantor trust processed a total of $11.6 billion in payments from AARP members in 2019—the investment gains quickly add up.[31]
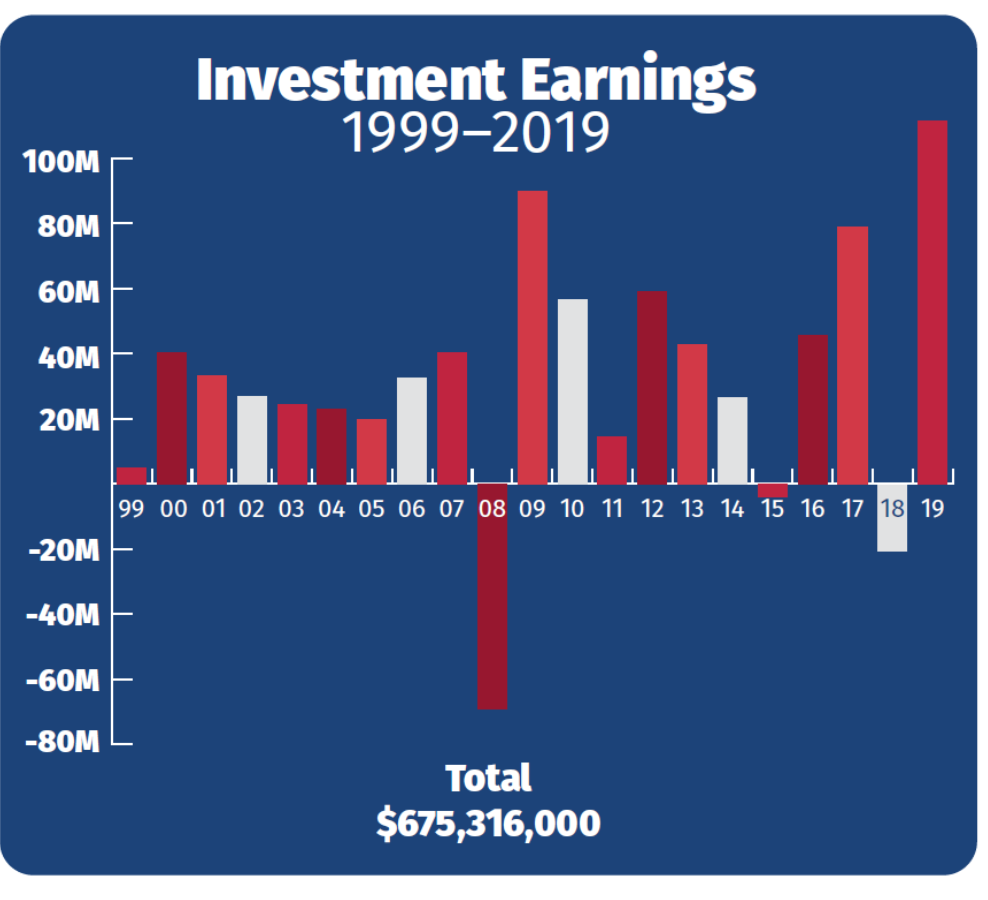
Over the past two decades, AARP has made more than half a billion dollars—$675.3 million, to be exact—investing seniors’ premium payments via its grantor trust.[32] In only three years—during the market crash in 2008, in 2015, and in 2018—did AARP lose money in its investments made via the grantor trust.[33] On average, however, the organization made $32.2 million per year via these investments—much, but not all, of which came from premium payments made by members for UnitedHealth Group insurance.[34]
Extravagant Compensation & Benefits
In 2019, AARP paid its CEO, Jo Ann Jenkins, a total of $1,409,028 in salary, benefits, and other compensation.[35] The payout continued a long-standing tradition of the organization spending large sums on executive compensation. In 2006, AARP paid its then-CEO, Bill Novelli, over $2 million in compensation—this in a year when AARP suffered a nearly $26 million shortfall.[36] And when Novelli’s successor, Barry Rand, retired on September 1, 2014, he received nearly $1.7 million in compensation—after working for only eight months out of the year.[37]
But the high compensation levels do not stop with AARP’s CEO. Of a total of 13 AARP other officers, key employees, and other highly compensated staff listed on the organization’s 2019 Form 990 filed with the Internal Revenue Service, all received more than $450,000 in total compensation.[38] These figures only include the salaries and compensation for key executives for which the IRS requires disclosure. By definition, it does not include other AARP executives, or executives of the AARP Foundation, a separate legal entity with its own salaried officers and staff.
According to its IRS filing, in 2019 over 60% (1,215) of AARP’s total employees (2,007) received reportable compensation from the organization in excess of $100,000.[39] Dividing the organization’s total spending on employee compensation in 2019 ($342,869,535) by its number of employees (2,007) reveals that AARP employees received an average of $170,836.84 in salaries, benefits and other compensation.[40]
By comparison, in 2019 the average senior citizen received $1,461 in monthly Social Security benefits.[41] That $17,532 total annual benefit represents just over one-tenth the total compensation provided to the average AARP employee. To put it another way, in 2019 AARP paid nearly $43 million more in compensation to its employees than the organization itself received in dues from its members—and over $217 million more than AARP spent giving grants to other organizations.[42]
Furthermore, AARP officials have admitted that the organization’s overall revenue totals—including “royalty fees” obtained by selling seniors AARP-branded products—impact the compensation decisions of its senior executives. As one anonymous staffer told the Washington Post, “Revenues are very important. You have to make your numbers.”[43] In other words, if AARP does not receive enough “royalty fees” from selling products to its members, its CEO and other senior executives could lose bonuses or other financial compensation.
Medigap: The AARP Cash Cow
As noted above, AARP has received a stunning amount of revenue—an estimated $6.7 billion—from UnitedHealth Group since 2007. However, the organization does not delineate how much of said revenue comes from each of the three types of plans UnitedHealth sells: Medicare Advantage plans, Medicare Part D prescription drug coverage, and Medigap supplemental coverage. A 2011 report by the House Ways and Means Committee found that AARP brands held dominant market shares in all three categories.[44]
However, among the three forms of coverage, AARP receives a flat annual “royalty fee” from UnitedHealth covering the sale of its AARP-branded Part D and Medicare Advantage plans, regardless of the plans’ enrollment. Conversely, for Medigap coverage, AARP receives a “royalty fee” from UnitedHealth equal to 4.95% of premium revenues paid.[45]
This percentage-based “royalty fee” gives AARP a strong financial incentive to aggressively market, sell, and renew as many Medigap policies as possible—and the most expensive policies at that—because AARP receives nearly five cents for every additional premium dollar its members pay to UnitedHealth. Perhaps as a result, some of AARP’s own members have considered these revenues not so much “royalty fees” as “kickbacks.”[46]
That 4.95% “royalty fee” represents a sizable share of premium dollars paid. To put the figure into perspective, it exceeds the current profit margins of five publicly held health insurers (Anthem, Centene, Humana, Molina, and Triple-S Management), and approaches the profit margin of the other (UnitedHealth Group).[47]
More to the point, AARP’s “royalty” margins come even though the organization bears no financial risk. The organization often notes that it is “not an insurance company”—a very true statement.[48] Insurers like UnitedHealth, Anthem, and Humana must take on financial risk, and can lose money in down markets or under turbulent circumstances. For instance, insurers lost an estimated $2.7 billion selling individual insurance policies in 2014, the first year of Obamacare’s Exchanges, and even more in the year following.[49] By contrast, however, AARP bears no risk, such that it cannot lose—all it has to do is sign up individuals and watch the cash roll in by the billions.
To give some sense of the questionable propriety of AARP’s current arrangements with UnitedHealth, in 1997 the group abruptly abandoned its plans for a percentage-based “royalty fee” for selling Medicare managed care plans (the precursor to Medicare Advantage).[50] At the time, government officials believed the arrangement potentially violated the Anti-Kickback Statute, which imposes criminal penalties for anyone who gives a “thing of value” in exchange for referrals of individuals to federal health programs.[51] The then-head of the agency that runs Medicare, Bruce Vladeck, also reportedly thought the arrangement could cause AARP to “lose its credibility as an advocate for its members if it endorses HMOs [Health Maintenance Organizations] and receives a financial reward.”[52]
Even though potential concerns that the arrangement violated a criminal statute led AARP to abandon its plans for percentage-based “royalties” to sell Medicare Advantage coverage, the organization has retained that approach when selling Medigap coverage—and has profited handsomely from it. Publicly available information suggests that most of AARP’s revenue from UnitedHealth comes via the sale of Medigap plans.
According to UnitedHealth’s annual filing with the Securities and Exchange Commission, in 2019 the insurer enrolled 4,500,000 individuals in Medicare supplemental (i.e., Medigap) plans.[53] Multiple surveys suggest that the average Medigap policy costs seniors approximately $150 per month, or around $1,800 per year.[54] Based on an average Medigap premium of $1,800 annually, UnitedHealth received about $7-8 billion in total Medigap premiums from its members in 2019. AARP’s 4.95% share of that sum would total roughly $350-400 million.[55]
Again, these numbers represent approximations, because AARP does not disclose the amount of money it receives from selling various health insurance policies—and since 2018, does not disclose the exact sum it receives from UnitedHealth at all. But it strongly suggests that the majority of the more than $600 million it receives from UnitedHealth in “royalty fees” comes from the sale of Medigap plans. It also suggests that AARP made far more money selling Medigap insurance to its members than the $300 million it received in membership dues.[56]
Financial Conflicts—And Secret Lobbying Campaigns
The percentage-based “royalty” formula gives AARP strong financial incentives to maximize enrollment in Medigap coverage. Whereas an additional participant in AARP-branded Part D plans or Medicare Advantage coverage provides no financial benefit to the organization, AARP’s bottom line benefits with every new person it can get to sign up for Medigap coverage. Likewise, AARP also benefits financially when it can entice individuals to sign up for more expensive Medigap policies, because it receives a percentage of every additional premium dollar seniors pay.
Even a former AARP chief executive has admitted that the organization faces financial conflicts regarding its insurance ties. In 2012, Bill Novelli, AARP’s CEO from 2001 through 2009, said that “it’s fair to say that AARP does have a financial interest in Medigap insurance because it’s a significant revenue raiser for them. If Medigap were somehow reduced, then AARP would have a financial reduction.”[57]
That financial conflict played out in 2011, when AARP secretly lobbied against changes to Medigap insurance—without disclosing its financial conflicts to Congress. At the time, lawmakers were considering changes to Medigap insurance that would have created a catastrophic cap on expenses in traditional Medicare, while requiring seniors purchasing Medigap coverage to pay deductibles and co-payments.[58] In total, these changes would have lowered Medigap premiums so dramatically that most seniors would have saved significant sums, even after paying additional co-payments out-of-pocket. A Kaiser Family Foundation analysis concluded that nearly four in five seniors (79%) would benefit financially, to the tune of an average savings of $415 per year.[59]
But if seniors win, saving money by paying smaller premiums, AARP loses—to be exact, it loses 4.95 cents of every dollar seniors save by paying lower Medigap premiums. Perhaps unsurprisingly, then-CEO Barry Rand wrote to a congressional “supercommittee” established to suggest changes to entitlement programs in October 2011, stating that AARP opposed any changes to Medicare or Medigap.[60] But in setting out AARP’s position on Medigap reform, Rand “did not mention AARP’s dominant role in the Medigap market,” or for that matter the organization’s financial incentive—to say nothing of the financial incentives associated with Rand’s own compensation—to keep Medigap premiums high and maximize AARP’s “royalties.”[61]
Another former AARP executive, Marilyn Moon, admitted that the organization had “an inherent conflict of interest,” because AARP “ended up becoming very dependent on sources of income.”[62] With respect to the stealthy way AARP tried to thwart Medigap reform, Moon noted:
Any way you look at changes in Medigap that people are talking about, I think it’s good for beneficiaries, and anybody who is opposing that who claims they are looking out for beneficiaries, you have to wonder why.[63]
Of course, in the case of AARP, one doesn’t have to wonder: The financial conflicts are obvious to everyone who understands how its “royalty fee” arrangements operate.
Discriminating Against the Most Vulnerable
The congressional supercommittee did not represent the only time in which AARP betrayed the principles to which the organization purportedly adheres. The drug pricing “negotiation” bill AARP supports would import other countries’ discrimination against their most vulnerable citizens, devaluing Americans with disabilities in the process.
The legislation, H.R. 3, would require the Department of Health and Human Services (HHS) to “negotiate” the prices of at least 50, and up to 250, brand-name prescription drugs. These “negotiated” prices would apply to Medicare, but private insurance companies like UnitedHealth could also adopt them for plans they sell.
While the legislation calls for a process of “negotiation” between the federal government and pharmaceutical manufacturers, it does so with a pre-determined outcome. Under the bill, the federal government could pay no more than 120% of the average price of drugs in six countries: Australia, Canada, France, Germany, Japan, and the United Kingdom. Companies that refuse to participate in the “negotiation” process would face excise taxes of up to 95%. Because of those onerous penalties, the Congressional Budget Office concluded that all companies “would either participate in the negotiation process or pull a particular drug out of the U.S. market entirely.”[64]
Experts agree that H.R. 3 would reduce access to new drugs and therapies, by reducing incentives for innovation. The Congressional Budget Office concluded that the legislation would result in approximately eight fewer drugs coming to market within its first decade, and 30 fewer drugs over its subsequent decade, or roughly ten percent.[65]
Other estimates show a far greater impact of foreign price controls on drug development. In 2019, the Council of Economic Advisers concluded that H.R. 3 would reduce drug development by one-third, resulting in the introduction of 100 fewer drugs over a decade.[66] These potential drugs not developed represent diseases—and patients—not cured, lives not improved, and potentially dangerous pathogens like COVID-19 not addressed.
By using foreign price controls as a backstop for drug “negotiation,” H.R. 3 would also import these countries’ discrimination against the most vulnerable. Several of the countries specified in H.R. 3 use the Quality-Adjusted Life Year (QALY) metric to determine payment levels. For instance, Britain’s National Institute for Health and Care Excellence assesses the cost of a drug using the QALY formula to determine whether and how the National Health Service will cover the treatment.[67]
But the QALY metric presupposes higher values for an additional year of life for people in “normal” health than for a person with an injury or disability, discriminating against individuals with disabilities in potentially illegal ways. A report by the National Council on Disability regarding QALYs noted that “one of the most prominent attempts to utilize QALYs in a state-run insurance program was found to violate the Americans with Disabilities Act.”[68]
For these reasons, a consortium of disability groups wrote to congressional leaders in September 2019, shortly after H.R. 3’s introduction, asking them to ban use of the QALY metric. Their letter noted that “the QALY is a discriminatory measure based on the idea that disabled lives are less valuable than non-disabled lives,” and stated the consortium “is very concerned that” the price-setting provisions in H.R. 3 “effectively import a QALY-based and discriminatory system from abroad. These systems are discriminatory against people with disabilities and do not have a place in the United States health care system.”[69]
Following that letter, the congressional committees modified H.R. 3 slightly. The version of H.R. 3 passed by the House in December 2019 requires HHS to consider the effects of drugs on specific populations, including individuals with disabilities, and prohibits the Department from treating the life of elderly or disabled individuals as worth less than younger and less vulnerable populations.[70]
However, the bill’s very next sentence effectively nullifies the provisions inserted to protect individuals with disabilities. That sentence states that “nothing” in the requirements on HHS regarding vulnerable populations “shall affect the application or consideration of an [average international market] price for a selected drug.”[71] In other words, the foreign price controls still apply to the “negotiation” process, which would in the words of the disability consortium “effectively import a QALY-based and discriminatory system from abroad.”
Despite the serious concerns raised by disability groups that the legislation discriminates against the most vulnerable, AARP still endorsed H.R. 3.[72] Both AARP members and Congress should ask why the organization supports legislation that devalues individuals with disabilities, and whether the potential benefits to its insurance partner UnitedHealth—which under the bill could utilize the lower drug prices “negotiated” by the federal government to increase its own profits—have anything to do with AARP’s policy stance.
A Compromised Organization
The sordid history of AARP’s dealings in Washington—the legally questionable way it has conducted its business to obtain billions of dollars in profits, the secretive way in which AARP lobbied to kill Medigap reform without informing lawmakers of its financial conflicts, and its more recent history of supporting legislation that devalues individuals with disabilities—demonstrate how its revenue sources have compromised the integrity of its policy positions.
As one observer noted several years ago: “Either you’re a voice for the elderly or you’re an insurance company—choose one.”[73] Sadly, AARP has largely chosen the latter course of action, becoming reliant on UnitedHealth for a significant share of its revenue, even as it tries to portray itself as the former.
Congress has investigated AARP and its financial dealings on more than one occasion. It should do so again, and determine whether any legislative and/or regulatory actions—requiring AARP to disclose its financial conflicts to seniors when they apply for Medigap coverage, for instance—can protect AARP’s members from the organization’s unholy alliance with UnitedHealth Group.
This report was originally published by American Commitment.
[1] Milt Freudenheim, “AARP Dropping Plans for Royalties in a Health Program,” New York Times April 19, 1997, https://www.nytimes.com/1997/04/19/business/aarp-dropping-plans-for-royalties-in-a-health-program.html; “Can You Trust the AARP?” New York Times May 20, 1996, https://www.nytimes.com/1996/05/20/opinion/can-you-trust-the-aarp.html; Jerry Markon, “AARP Lobbies Against Medicare Changes That Could Hurt Its Bottom Line,” Washington Post December 4, 2012, https://www.washingtonpost.com/politics/aarp-lobbies-against-medicare-changes-that-could-hurt-its-bottom-line/2012/12/03/aa3e509e-3a8c-11e2-b01f-5f55b193f58f_print.html.
[2] AARP Inc., 2019 Form 990, https://www.aarp.org/content/dam/aarp/about_aarp/annual_reports/2020/2019-aarp-form-990-public-disclosure.pdf, p. 1.
[3] Ibid.
[4] AARP Inc., Forms 990, 2009 through 2019. While only the 2017, 2018, and 2019 statements are visible on the organization’s website, https://www.aarp.org/about-aarp/company/annual-reports/, all copies of the AARP Forms 990 are available through a ProPublica database, https://projects.propublica.org/nonprofits/organizations/951985500.
[5] Ibid.
[6] Fortune 500, 2021, https://fortune.com/fortune500/2021/search/?f500_industry=Health%20Care%3A%20Insurance%20and%20Managed%20Care. Health insurers include UnitedHealth Group, Anthem, Centene, Humana, Molina Healthcare, and Triple-S Management. The other Fortune 500 company listed under “Insurance and Managed Care,” Magellan Health, focuses on managing behavioral health issues, as opposed to selling health insurance products to individuals and/or employers.
[7] AARP Inc., 2019 Consolidated Financial Statements, March 17, 2020, https://www.aarp.org/content/dam/aarp/about_aarp/annual_reports/2019/fiscal-2019-consolidated-financial-statements.pdf, p. 6.
[8] Ibid.
[9] Ibid.
[10] AARP Inc., Consolidated Financial Statements, 2000 through 2019. While only the 2017, 2018, and 2019 statements are visible on the organization’s website, https://www.aarp.org/about-aarp/company/annual-reports/, Internet searches for “AARP Consolidated Financial Statements” and the year in question reveal that prior years’ statements remain online (albeit not linked from the AARP homepage). Links to specific years’ statements are provided in citations below.
[11] Ibid.
[12] Ibid.
[13] Ibid.
[14] Ibid.
[15] Ibid.
[16] AARP Inc., 2008 Consolidated Financial Statements, March 30, 2009, https://assets.aarp.org/www.aarp.org_/TopicAreas/annual_reports/assets/AARPConsolidatedFinancialStatements.pdf, pp. 4, 9. The 2008 financial statements represent the first instance in which AARP disclosed the percentage of total royalties coming from UnitedHealth Group. However, the 2008 statements also included data for the prior year period, making calculations for 2007 possible.
[17] AARP Inc., 2017 Consolidated Financial Statements, March 16, 2018, https://www.aarp.org/content/dam/aarp/about_aarp/about_us/2018/aarp-2017-audited-financial-statement.pdf, pp. 4, 11.
[18] Ibid.
[19] Ibid.
[20] 2008 through 2017 Consolidated Financial Statements.
[21] 2018 Consolidated Financial Statements. The relevant language previously appeared in the royalties section of the statements’ Summary of Significant Accounting Practices. The 2018 statements’ Summary of Significant Accounting Practices eliminates the discussion of royalties entirely. Compare pp. 8-13 of the 2017 Statements with pp. 8-13 of the 2018 Statements.
[22] 2008 through 2017 Consolidated Financial Statements.
[23] Chris Jacobs, “How AARP Made Billions Denying Care to People with Pre-Existing Conditions,” The Federalist October 11, 2018, https://thefederalist.com/2018/10/11/aarp-made-billions-denying-care-people-pre-existing-conditions/.
[24] 2018 Consolidated Financial Statements, pp. 14-15.
[25] Ibid.
[26] 2017 Consolidated Financial Statements, pp. 4, 11.
[27] 2018 Consolidated Financial Statements, p. 14.
[28] 2019 Consolidated Financial Statements, p. 15.
[29] 2008 through 2019 Consolidated Financial Statements.
[30] 2019 Consolidated Financial Statements, p. 20.
[31] Ibid.
[32] 2000 through 2019 Consolidated Financial Statements.
[33] 2008 Consolidated Financial Statements, p. 15; AARP Inc., 2015 Consolidated Financial Statements, March 17, 2016, https://www.aarp.org/content/dam/aarp/about_aarp/annual_reports/2016/2015-financial-statements-AARP.pdf, p. 14; 2018 Consolidated Financial Statements, p. 19.
[34] 2000 through 2019 Consolidated Financial Statements. While AARP has previously disclosed that most of its royalty fees come from UnitedHealth Group, AARP has never disclosed the precise percentage of grantor trust investment income attributable to policies sold by UnitedHealth.
[35] 2019 Form 990, p. 7.
[36] AARP Inc., 2006 Form 990, https://projects.propublica.org/nonprofits/display_990/951985500/2008_02_EO%2F95-1985500_990O_200612, pp. 1, 14.
[37] AARP Inc., 2014 Form 990, https://www.aarp.org/content/dam/aarp/about_aarp/annual_reports/2015-08/2014-IRS-Form-990-AARP.pdf, p. 10.
[38] 2019 Form 990, pp. 7-8.
[39] Ibid., pp. 1, 8.
[40] Ibid., pp. 1, 8.
[41] Social Security Administration, “Fact Sheet: 2019 Social Security Changes,” November 2018, https://www.ssa.gov/news/press/factsheets/colafacts2019.pdf.
[42] 2019 Form 990, p. 1; 2019 Consolidated Financial Statements, p. 6.
[43] Markon, “AARP Lobbies Against Changes.”
[44] House Ways and Means Committee, “Behind the Veil: The AARP America Doesn’t Know,” March 30, 2011, https://gop-waysandmeans.house.gov/UploadedFiles/AARP_REPORT_FINAL_PDF_3_29_11.pdf, Table 2, p. 9.
[45] Ibid., pp. 11-12.
[46] Gary Cohn and Darrell Preston, “AARP’s Stealth Fees Often Sting Seniors with Costlier Insurance,” Bloomberg December 4, 2008, https://www.bloomberg.com/news/articles/2008-12-04/aarp-s-stealth-fees-often-sting-seniors-with-costlier-insurance.
[47] 2021 Fortune 500.
[48] Lee Hammond, AARP President, Letter to the Editor, Wall Street Journal January 11, 2011, https://www.wsj.com/articles/SB10001424052748704415104576065993584399626.
[49] McKinsey, “Exchanges Three Years In: Market Variations and Factors Affecting Performance,” May 2016, https://healthcare.mckinsey.com/exchanges-three-years-market-variations-and-factors-affecting-performance.
[50] Freudenheim, “AARP Dropping Plans.”
[51] Ibid.; Section 1128B of the Social Security Act, 42 U.S.C. 1320a-7b.
[52] Freudenheim, “AARP Dropping Plans.”
[53] UnitedHealth Group, Inc, 2020 Form 10-K, March 1, 2021, https://info.uhg.com/content/dam/UHG/PDF/investors/2020/UNH-Form-10-K.pdf, p. 41.
[54] For instance, online broker eHealthInsurance found an average Medigap premium of $141 per month in 2018 and $152 per month in 2019 among its customers; see eHealthInsurance, “Medicare Index Report: Annual Enrollment Period for 2019 Coverage,” February 7, 2019, https://news.ehealthinsurance.com/_ir/68/20191/eHealth%20Medicare%20AEP%20Report.pdf, p. 2. Business Insider used a survey by HealthView Services to cite an average premium of $143 per month for Medigap Plan F, the most popular Medigap plan, in 2018; see Hillary Hoffower, “Medicare Isn’t Enough for Retirees—Here’s How Much Extra Coverage Costs in Every State, Ranked,” Business Insider June 17, 2018, https://www.businessinsider.com/how-much-medigap-plans-cost-every-state-ranked-2018-6. Another brokerage site quoted an average premium of $169.14 for Medigap Plan F in 2018, the fourth highest among the 10 types of Medigap plans surveyed; see Christian Worstell, “What Is the Average Cost of Medicare Supplement Insurance Plan F?” October 3, 2019, https://www.medicaresupplement.com/articles/average-cost-of-medicare-supplement-plan-f/.
[55] The precise numbers in question would equal $8.1 billion and $400.95 million, respectively. However, because these numbers are based on rough approximations of premiums, we have provided ranges above.
[56] 2018 Consolidated Financial Statements, p. 4.
[57] Markon, “AARP Lobbies Against Changes.”
[58] While the congressional “supercommittee” could not reach agreement in 2011 on a package of entitlement reforms, Congress did eventually enact modest changes to Medigap insurance. Section 401 of the Medicare Access and CHIP Reauthorization Act of 2015, P.L. 114-10, provided that beginning in January 2020, Medigap policies sold to new Medicare beneficiaries (i.e., those just turning 65) cannot provide coverage for the Medicare Part B deductible, a measure designed to reduce unnecessary utilization of the health care system.
[59] Kaiser Family Foundation, “Medigap Reforms: Potential Effects of Benefit Restrictions on Medicare Spending and Beneficiary Costs,” July 2011, https://www.kff.org/wp-content/uploads/2013/01/8208.pdf, Exhibit 2: Changes in Medicare Spending Per Beneficiary and Average Beneficiary Costs under Three Medigap Benefit Options, p. 6.
[60] Markon, “AARP Lobbies Against Changes.”
[61] Ibid.
[62] Cohn and Preston, “AARP’s Stealth Fees.”
[63] Markon, “AARP Lobbies Against Changes.”
[64] Congressional Budget Office, Letter to Rep. Frank Pallone regarding H.R. 3, October 11, 2019, https://www.cbo.gov/system/files/2019-10/hr3ltr.pdf, p. 14.
[65] Congressional Budget Office, Letter to Rep. Frank Pallone regarding H.R. 3, December 10, 2019, https://www.cbo.gov/system/files/2019-12/hr3_complete.pdf, p. 6.
[66] White House Council of Economic Advisers, “House Drug Pricing Bill Could Keep 100 Lifesavings Drugs from American Patients,” December 3, 2019, https://trumpwhitehouse.archives.gov/articles/house-drug-pricing-bill-keep-100-lifesaving-drugs-american-patients/.
[67] Nigel Edwards, Helen Crump, and Mark Dayan, “Rationing in the NHS,” Nuffield Trust Policy Brief #2, February 2015, https://www.nuffieldtrust.org.uk/files/2017-01/rationing-in-the-nhs-web-final.pdf, p. 8.
[68] National Council on Disability, “Quality-Adjusted Life Years and the Devaluation of Life with Disability,” Bioethics and Disability Series, November 6, 2019, https://ncd.gov/sites/default/files/NCD_Quality_Adjusted_Life_Report_508.pdf, p. 45.
[69] Consortium for Citizens with Disabilities, Letter to House Education and Labor, House Energy and Commerce, and House Ways and Means Committees regarding H.R. 3, September 24, 2019, http://www.c-c-d.org/fichiers/CCD-Letter-HR-3-Final-9.24.19.pdf.
[70] Compare proposed new Section 1194(d)(2) of the Social Security Act in H.R. 3 as introduced in the House during the 116th Congress on September 19, 2019, p. 25, with proposed new Section 1194(d)(2) of the Social Security Act in H.R. 3 as passed by the House on December 12, 2019, pp. 33-34. The version of H.R. 3 reintroduced for the 117th Congress on April 22, 2021 includes the language included in pp. 33-34 of the House-passed version from December 2019.
[71] Ibid.
[72] AARP, Letter to House Education and Labor, House Energy and Commerce, and House Ways and Means Committees regarding H.R. 3, May 7, 2021, https://www.aarp.org/content/dam/aarp/politics/advocacy/2021/05/may-2021-hr-3-endorsement-letter-050721.pdf.
[73] Dan Eggen, “AARP: Reform Advocate and Insurance Salesman,” Washington Post October 27, 2009, https://www.washingtonpost.com/wp-dyn/content/article/2009/10/26/AR2009102603392_pf.html.